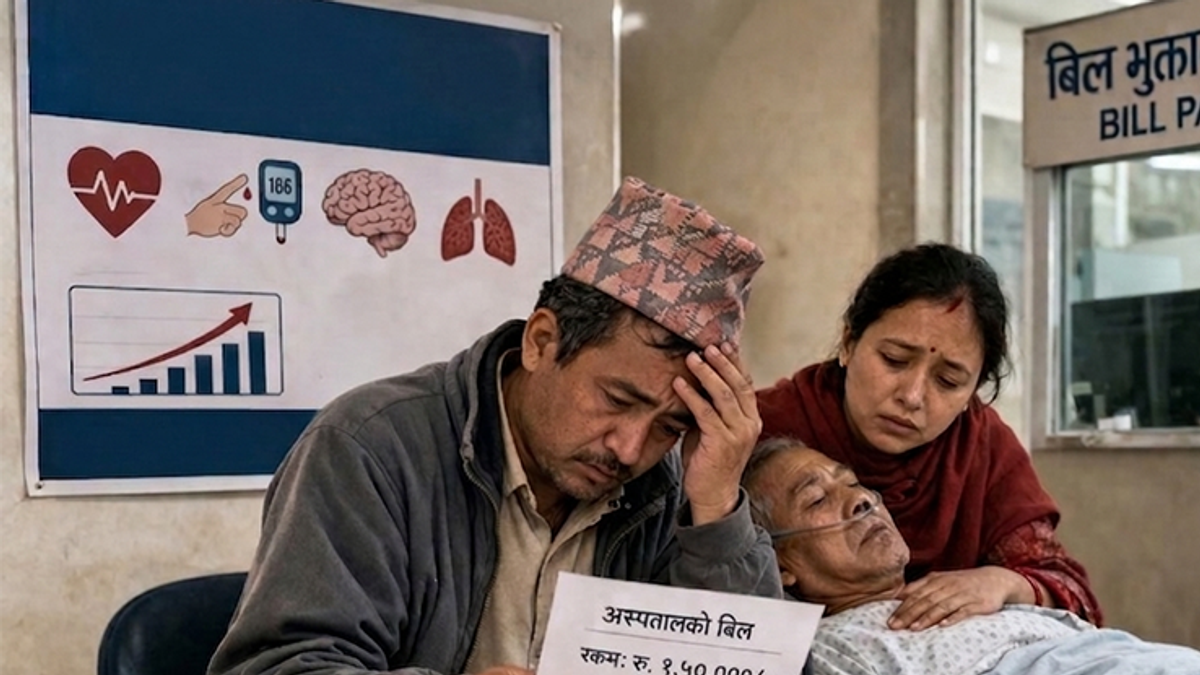
Citizens Confronting Street Life Due to Escalating Treatment Costs for Non-Communicable Diseases
News Summary
Produced by AI. Editorially reviewed.
- The incidence of non-communicable diseases is rapidly rising in Nepal, with over 193,000 annual deaths attributed to these illnesses.
- Kidney disease patients Hastimaya Limbu and Rambahadur Tamang have undergone kidney transplants but face severe financial hardship due to treatment costs.
- The government has implemented a multisectoral plan to prevent non-communicable diseases, yet greater emphasis appears placed on treatment over prevention.
March 30, Kathmandu – The life story of 55-year-old Hastimaya Limbu from Jhapa resembles a dramatic film. After her husband became unreachable, she single-handedly supported her two daughters and traveled to Oman in 2016 (2073 BS) for employment.
Life in Oman was extremely tough for Limbu. She worked continuously as a domestic worker from 5 a.m. to 11 p.m. daily. “I took care of cleaning, cooking, and laundry,” she recalled, “Working day and night left my body aching, and sometimes I had to take painkillers.”
Despite extreme heat, she drank only boiled water. The heavy workload caused her to suppress the urge to urinate, seriously affecting her health. She lost appetite, suffered severe back pain, and experienced persistent vomiting. One day, she fainted and was rushed to the hospital by her employer. There, she was shocked to learn both her kidneys had failed.
After four days of dialysis, her employer sent her back to Nepal. Returning amid the COVID-19 pandemic brought additional challenges—her health deteriorated due to the infection while undergoing dialysis.

Her struggle continued. Her sister was also prepared to donate a kidney, but was found to have gallstones and required gallbladder removal. Finally, in March 2023 (2080 BS), Hastimaya’s kidney transplant was successful. She shared, “I have spent over 6 million Nepali rupees for this.”
“At home, I had to cook meat dishes daily. Especially, the employer liked heavily salted meat,” she said. “I may have damaged my kidneys by eating salty meat.”
Currently, she visits Tribhuvan University Teaching Hospital periodically for follow-ups. “Now I depend on others to survive,” she said. “My monthly medication alone costs 15,000 rupees.”
Similar difficulties are faced by 52-year-old Rambahadur Tamang from Kavre. Living in rented accommodation in Kathmandu and supporting his family by daily wage labor, he would leave for work in the morning and return in the evening.
“When living alone, I did not feel like cooking. I ate market food morning and evening,” he admitted. “This affected my health.”
He pointed out that communities consuming readily available oily, salty, and junk food can experience deteriorating health.
Tamang developed fatigue, numbness, and worsening health. When critically ill and hospitalized, he was informed that his kidneys had failed. He spent several years on dialysis.
His son donated a kidney two years ago, successfully enabling a transplant, but the financial crisis pushed the family toward destitution.
“We used to consume large amounts of oil and junk food from the market,” he recalled. “That habit caused my kidney damage.”
The government provided 500,000 rupees in support for the transplant, but the cost of medicine and additional expenses exceeded that. “We had to sell land and property to cover treatment costs,” he revealed.
These incidents highlight the growing burden of non-communicable diseases. Public health specialist Dr. Kedar Baral stated, “Changes in lifestyle and diet have led to increased disease rates.”
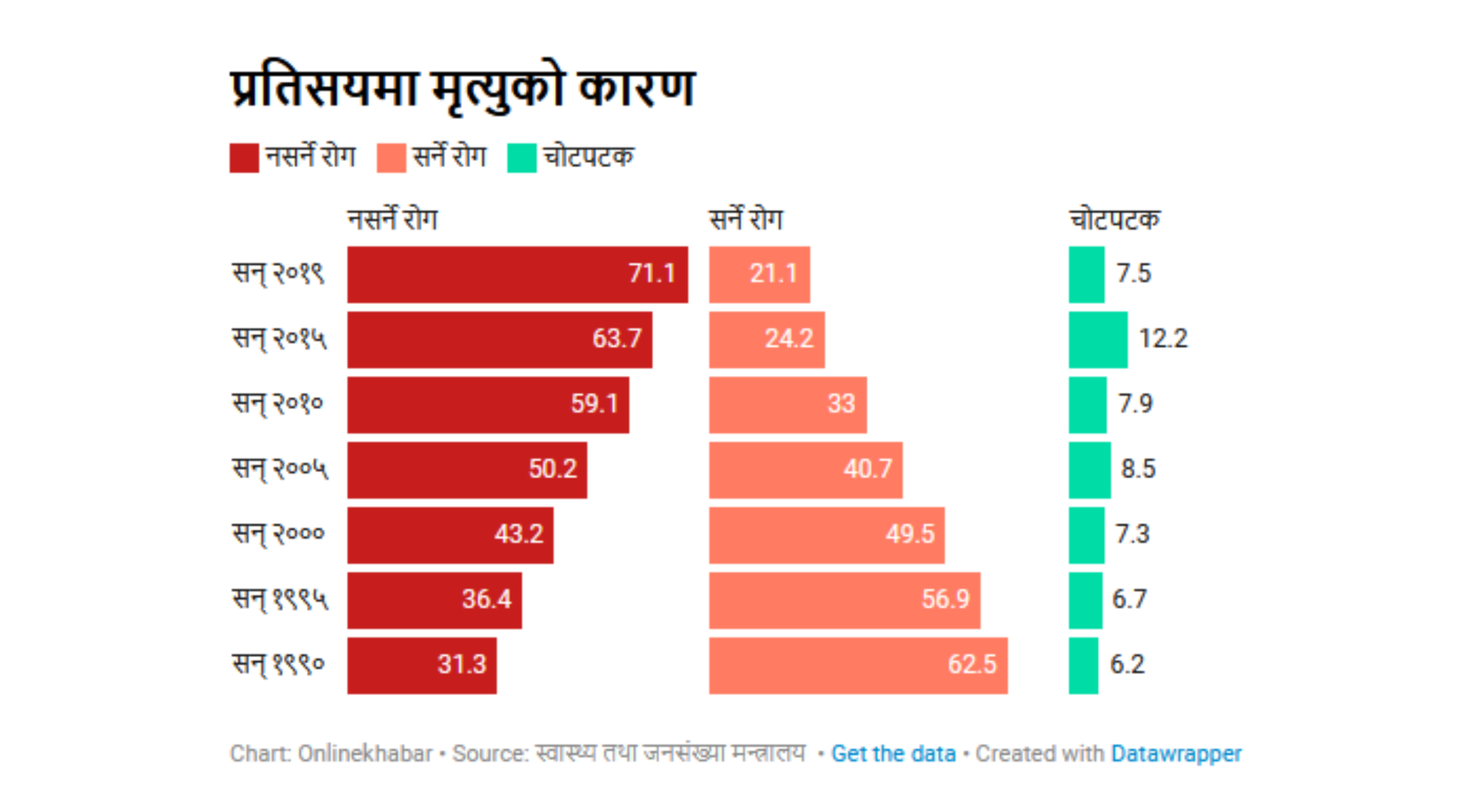
Experts note that dietary and lifestyle changes in recent years have elevated disease risks. While infectious diseases were the leading cause of death previously, non-communicable diseases have now become predominant.
Among Nepal’s top 10 causes of death, eight are non-communicable diseases. Board of Disease Statistics reports over 193,331 deaths annually due to these illnesses.
Cardiovascular diseases claim around 46,399 lives per year. Chronic respiratory diseases cause 40,792 premature deaths. Tumors and cancers account for 21,653 deaths annually. Other diseases also contribute thousands of fatalities each year.
Experts attribute primary causes to modern lifestyles and unhealthy dietary patterns. Seventy-one percent of mortality in Nepal results from these conditions.
Professor Dr. Madhusudan Subedi of Patan Academy of Health Sciences explained that the number of patients has surged rapidly in the last three decades. Previously, heavy physical labor was common, but dependence on motorcycles and scooters has increased now.
Treatment costs for non-communicable diseases are pushing many families into economic hardship, with over five hundred thousand people annually falling below the poverty line due to medical expenses.
According to Dr. Subedi, consumption of oily, processed, and fast foods has led to increased cases of heart disease, diabetes, and cancer.
“We think we are eating healthily, but pesticide-laden food harms our well-being,” he said.
Senior cardiologist Dr. Rajendra Koju observed that many foods available in markets contain excessive fats. Fried, salted, and frozen foods increase trans fats, posing long-term health risks.
Trans fats raise cholesterol, blood pressure, diabetes, and obesity risks, and increase vulnerability to heart, kidney, and brain diseases.
Research on fatty foods shows increased use of trans fats in biscuits, cookies, samosas, chips, cakes, pizzas, momos, and other commonly consumed items.
The Non-Communicable Disease Costs for the Vulnerable Have Doubled in Five Years
Government data shows that the number of impoverished citizens receiving assistance through expensive medicine programs has doubled over five years. Patients with cancer, heart disease, dialysis, and kidney transplants have increased.
Expenses have also doubled within this period—from 214 million rupees in fiscal year 2020/21 to 442 million in 2023/24.
This service is also being provided through the Health Insurance Board, with over 46,000 poor patients receiving care via insurance.
Analysis by the Department of Health shows that hypertension, diabetes, and cancer patients rely heavily on insurance-provided services. Non-communicable diseases account for half of these claims.
Experts like Malla emphasize the rising patient numbers and financial burdens on the health system due to these chronic illnesses.
Citizens bear approximately 40% of their own treatment expenses. Kidney disease, diabetes, cancer, hypertension, and heart diseases impose long-term economic strain.
Health economist Ghanshyam Gautam emphasizes that prevention is more cost-effective than treatment and urges government investment in prevention programs.
Smoking, poor diet, physical inactivity, obesity, and stress exacerbate these issues.
Government data reveals that the average health service use costs roughly 27,000 rupees, potentially causing chronic financial hardship.
Nepalis tend to focus on treatment only after falling ill. Cardiologist Dr. Bhagwan Koirala advocates for mandatory prevention and regular screening to avoid disease onset.
Dr. Koirala highlights the need for greater government investment in prevention over treatment.

The Disease Web Spread by Pollution and Junk Food
Experts state that smoking, poor diets, physical inactivity, obesity, and stress are increasing non-communicable diseases.
Dr. Rajendra Koju, senior cardiologist at Dhulikhel Hospital, reports heart attacks occurring at younger ages, primarily due to smoking.
Cardiovascular diseases also elevate stroke risk. Neurosurgeon Dr. Rajiv Jhakri predicts stroke may become a leading cause of death over the next 8-10 years.
Chest disease specialist Dr. Raju Pangeni notes that chronic respiratory diseases affect over 90% of patients, including COPD, asthma, and bronchitis.
According to Dr. Pangeni, asthma is prevalent among those over 40, with air pollution and smoking as main causes.
“Environmental pollution and unhealthy diets weaken immunity,” she said.
Cancer specialist Dr. Vivek Acharya links poor diet, unbalanced routines, and unhealthy lifestyles to increased cancer risks.
Packaging, junk, and processed foods are major contributors to cancer incidence.
Excessive meat, junk, and salty food intake raise digestive tract cancer risks, Dr. Acharya added.
“Sedentary lifestyles and low physical activity increase obesity and cancer risk,” he explained.
Previously, Nepalis primarily ate home-cooked meals, but there has been a surge in fast and processed food consumption now.
Gastroenterologist Dr. Bhupendra Kumar Basnet explained that heavy oil use in many foods increases digestive problems and cancer risks.
Chemical additives also negatively affect health.
Late diagnosis of digestive diseases complicates treatment and increases mortality.
Kidney disease poses another significant public health challenge, with diabetes, hypertension, and obesity driving its rise.
Kidney specialist Dr. Rishikumar Kafle stated that kidney failure requires transplantation or dialysis. However, transplantation is not accessible to all, leaving many dependent on lifelong dialysis—a major challenge.
Kidney disease patients increase by approximately three thousand annually. Thousands await transplantation, but only about 200 surgeries occur yearly.

Government’s Treatment-Focused Policy Overshadows Prevention Efforts
The Ministry of Health and Population reports that non-communicable diseases are spreading like an epidemic. A multisectoral prevention program covering 2021-2025 has been implemented, with a new 2026-2030 action plan underway.
This plan aims to reduce premature deaths from heart disease, cancer, diabetes, and chronic illnesses by 33%.
However, active involvement from all levels and bodies is necessary for success.
Major factors contributing to non-communicable diseases lie outside the health sector as well, including pollution, waste management, pesticides, and chemical exposure.
The previous plan incorporated a multisectoral approach but lacked effective implementation. The government now plans to coordinate policies, resources, and programs more clearly.
Dr. Bikash Devkota emphasizes that not only the health sector but other sectors must reduce factors adversely affecting health.
Public health expert Dr. Kedar Baral noted that since non-communicable diseases are linked to lifestyle, lifestyle improvements are essential. “The government focuses more on treatment, but prevention needs greater efforts,” he stated.
Dr. Sharad Bant added that the health sector alone cannot control non-communicable diseases; intersectoral collaboration is mandatory. He cited weak policy formulation and implementation.
Dr. Rita Thapa described non-communicable diseases as a spreading epidemic, attributing it largely to lifestyle and habits.

“Children consume tobacco products, parents feed them junk food, physical activity declines, and stress increases,” said Dr. Thapa.
She stated that the government spends more on treatment than prevention, with too little attention on prevention.
According to Thapa, healthy lifestyle education should begin at school, as adolescent smoking and junk food consumption start early.
While developed countries have gained control over these diseases, Nepal—as a developing country—is witnessing a growing epidemic of non-communicable diseases.
Medical sociologist Madhusudan Subedi suggests the government increase investments in disease prevention, screening, and awareness programs.
Dr. Das indicated smoking, unhealthy diets, and sedentary lifestyles as major causes, recommending increased taxation on these behaviors.
Health economist Gautam argues that prevention investment is more cost-effective and beneficial long-term compared to treatment.